CoQ10 deficiency is broadly divided into primary and secondary types. Coenzyme Q10 is a vitamin-like substance that plays a key role in human cell metabolism. It is not quite a vitamin, though, because we humans can synthesize Coenzyme Q10.

The Mayo Clinic reference values for plasma CoQ10 concentrations are from 0.43 to 1.52 mg/L. The CoQ10 researcher Dr. William Judy found plasma CoQ10 levels below 0.6 mg/L to be worrisome. He thought that normal healthy adults should have plasma CoQ10 levels of at least 0.8 mg/L and preferably 1.0 mg/L..
However, once we pass into middle age and into our senior years, our ability to synthesize the substance declines with increasing age [Kalén 1989]. As a consequence, CoQ10 supplementation is necessary. It is not possible to make up for declining CoQ10 bio-synthesis simply by eating more or more wisely [Judy 2018].
Coenzyme Q10 is essential for cellular ATP energy generation. In addition, it is a major lipid-soluble antioxidant. Because it is so important in cell metabolism, insufficient bio-synthesis of Coenzyme Q10 is associated with mitochondrial dysfunction and increased oxidative stress and, as a result, with a number of medical conditions [Judy 2018].
Primary CoQ10 Deficiency
Mantle et al [2022, 2022] have written overviews of both primary and secondary deficiency conditions. Primary CoQ10 deficiency is a relatively rare condition. It results from mutations in genes involved in the CoQ10 biosynthesis pathway. At least 10 genes are required for the biosynthesis of functional Coenzyme Q10. A mutation in any one of these ten genes can result in a deficit in CoQ10 status. Primary CoQ10 deficiency has been estimated to affect approximately 120,000 patients worldwide [Mantle 2023].
Secondary CoQ10 Deficiency
Secondary CoQ10 disorder is the more frequent deficiency condition. It may occur for a variety of reasons [Mantle 2022]:
- aging
- oxidative-stress-induced reduction of CoQ10
- effects of pharmacological agents such as statins
- mutations in genes not directly related to the synthetic pathway
Mitochondrial Dysfunction as a Result of Primary CoQ10 Deficiency
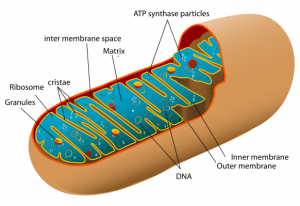
Mitochondria are organelles in the cytoplasm of cells. The mitochondria are sometimes called the powerhouses of the cells. Mitochondria produce the ATP, the main energy molecules in the cells.
Primary CoQ10 deficiency patients suffering from mitochondrial dysfunction may respond well to oral CoQ10 supplementation. However, the condition must be recognized sufficiently early. CoQ10 supplementation will be too late if critical organs such as the kidney or the nervous system have begun to suffer damage. Often, only minimal recovery will be possible [Mantle 2023].
CoQ10 Supplementation for Secondary CoQ10 Deficiency
Mantle et al [2022] have reviewed reports of reduced blood CoQ10 concentrations in the following groups of patients:
- Heart failure patients
- Chronic kidney disorder patients
- Non-alcoholic fatty liver disease patients
- Type 2 diabetes patients
- Parkinson’s disease patients
- Fibromyalgia patients
- Breast cancer patients
- Periodontal disease patients
CoQ10 Adjuvant Treatment of Heart Failure Patients
Can supplementation with Coenzyme Q10 result in significant clinical benefit? Mantle et al show that the best documented secondary CoQ10 deficiency disorder in which CoQ10 supplementation provides significant patient benefit is heart failure. They refer to nearly 30 randomized controlled trials of CoQ10 adjuvant treatment of heart failure patients that have reported significant patient benefit [Mantle 2015].
CoQ10 Supplementation of Patients with Other Conditions
Mantle et al [2022] cite evidence from randomized controlled trials that supplementary Coenzyme Q10 can improve blood glucose control, liver function, and renal function in patients with type 2 diabetes, non-alcoholic fatty liver disease, and chronic kidney disorder, respectively.
Conclusion: CoQ10 Deficiency Status
CoQ10 deficiency status can occur for a variety of reasons:
- Impaired CoQ10 biosynthesis
- Insufficient dietary intake
- Excessive utilization of Coenzyme Q10
There is much individual variability in the biosynthesis and dietary uptake of Coenzyme Q10. That said, ideally, a normal healthy adult should have a blood CoQ10 concentration of at least 1.0 mg/L [Judy 2018].
For adults with heart failure, a plasma CoQ10 level greater than 2.5 mg/L is required [Langsjoen 2014].
For adults with neurodegenerative disease, plasma CoQ10 levels greater than 3.5 mg/L are thought to be needed for a beneficial therapeutic effect [Langsjoen 2014].
Note: Absorption and bioavailability depends upon the formulation. All CoQ10 products are not absorbed equally well [Mantle & Dybring 2020].
It is important to find a CoQ10 product with documented evidence for its absorption and bioavailability [Lopez-Lluch 2019].
Sources
Judy WV. Coenzyme Q10: The Substance That Powers Life: An Insider’s Guide to Coenzyme Q10. Available from amazon.com. ISBN: 978-87-7776-186-7.
Kalén A, Appelkvist EL, Dallner G. Age-related changes in the lipid compositions of rat and human tissues. Lipids. 1989 Jul;24(7):579-84.
Langsjoen PH, Langsjoen AM. Comparison study of plasma coenzyme Q10 levels in healthy subjects supplemented with ubiquinol versus ubiquinone. Clin Pharmacol Drug Dev. 2014 Jan;3(1):13-7.
López-Lluch G, Del Pozo-Cruz J, Sánchez-Cuesta A, Cortés-Rodríguez AB, Navas P. Bioavailability of coenzyme Q10 supplements depends on carrier lipids and solubilization. Nutrition. 2019 Jan;57:133-140.
Mantle D, Millichap L, Castro-Marrero J, Hargreaves IP. Primary Coenzyme Q10 Deficiency: An Update. Antioxidants (Basel). 2023 Aug 21;12(8):1652.
Mantle D, Turton N, Hargreaves IP. Depletion and Supplementation of Coenzyme Q10 in Secondary Deficiency Disorders. Front Biosci (Landmark Ed). 2022 Dec 19;27(12):322.
Mantle D, Dybring A. Bioavailability of Coenzyme Q10: an overview of the absorption process and subsequent metabolism. Antioxidants (Basel). 2020 May 5;9(5):386.
Mantle D. Coenzyme Q10 and cardiovascular disease: an overview. British Journal of Cardiology. 2015;22:160.
Mayo Clinic Staff. Coenzyme Q10, Total, Plasma. Mayo Clinic. 2023. Retrieved from
https://www.mayocliniclabs.com/test-catalog/overview/63148#Clinical-and-Interpretive
The information presented in this review article is not intended as medical advice and should not be used as such.







Leave A Comment