The entire glucose metabolism is a series of energy demanding processes. Without adequate Coenzyme Q10 levels, diabetics will struggle to power these processes.
Do diabetics need a Coenzyme Q10 supplement? Good question. Answer: well, yes, diabetics have a heart muscle that constantly needs energy, so they too need to make sure that they are getting enough Q10. That seems logical enough. We know that the Q10 is so essential in the energy production process at the cellular level. While I was thinking about this question, Dr. William Judy of the SIBR Research Institute made an interesting observation that I will pass on here.
Glucose metabolism requires energy
Dr. Judy, whose education and experience is in physiology and bio-physics, made the following points to me (5):
- The glucose in the foods we eat is our main source of energy; the glucose is used to produce energy in our bodies in the form of ATP (adenosine triphosphate).
- The handling of glucose in the body is done by several active processes that, themselves, require energy, and, actually, taken together these processes require more energy than exercising requires.
- Glucose in food is absorbed in our intestines and transferred into the blood through energy dependent processes.
- To get the glucose from the blood to the cells, our cells are helped by the hormone insulin, which increases the permeability of absorption cells and other body cells, thereby allowing the glucose to be pumped into these cells through processes requiring energy.
- Our bodies store a small amount of extra glucose in the muscles and in the liver as glycogen. This storage process requires energy.
- When more glucose is needed, the glycogen is hydrolyzed to glucose and is released back into the blood. This allows a rapid energy burst in the onset of exercise.
- In our cells, the glucose is converted to energy in the form of ATP. In this process, Q10 is essential, and, when the cell temperature drops, this process is significantly reduced.
- In our kidneys, the reabsorption of glucose is done by active transport. which requires energy.
The important thing to notice, said Dr. Judy, is that all of these processes require energy.
Coenzyme Q10 deficiency can affect the glucose balance
Suddenly, it is clear that a deficiency of Q10 caused by long-term statin therapy can induce energy starvation at the cellular level and can ultimately affect the glucose balance in the body.
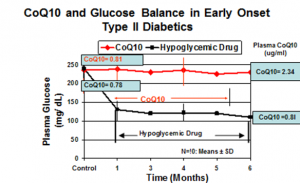
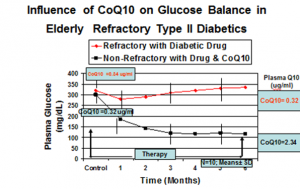
Dr. Judy has data that show that the body is not able to maintain glucose balance in older type II diabetics when the blood Q10 concentration is reduced to below 0.35 micrograms per milliliter. These patients become refractory to their hypoglycemic drugs. His data also show that glucose balance is vastly improved when Q10 supplementation raises plasma Q10 levels in refractory type II diabetics.
Not just insulin sensitivity and insulin secretion at fault
Dr. Judy said that there is more to the body’s ability to handle glucose than just insulin sensitivity and insulin secretion.
Why did he make that comment about insulin sensitivity and insulin secretion?
Finnish statins-diabetes study
He had been reading the report on the Finnish statins-diabetes study published in the journal Diabetologia in March 2015, in which the following points were made (1):
- Statin treatment increased the risk of type 2 diabetes by 46%, which the authors of the study attributed to decreases in insulin sensitivity and insulin secretion.
- Atorvastatin and Simvastatin are the two major statins that induced the increased risk of Type II diabetes. They are also the same statin drugs that induce the greatest reduction in CoQ10 synthesis in the body.
- There are dosage effects and age effects on the increased risk of developing Type II diabetes while taking statin medications. Higher statin doses and greater age in patients are more likely to induce refractory diabetes.
- The authors of the Finnish study focused on the reduction of insulin sensitivity and to the reduction of insulin secretion as the mechanisms for the increased risk of developing Type II diabetes. And, the data presented in the Finnish study do support this conclusion.
Coenzyme Q10’s effect on the glucose metabolism
However, as stated above, Dr. Judy thinks that there are other mechanisms that may be involved as well. Does Q10 affect glucose balance in the body, he asks? And his answer is that it has to. All of the processing of glucose in humans is done by active mechanisms that require energy.
Low Q10 levels and cellular energy starvation
When the Q10 level is low, there is cellular energy starvation, and there will be reduced glucose balance.
Based on the results of studies done in the late 1980’s and early 1990’s, Dr. Judy has come to the following conclusions:
- In normal individuals with normal plasma CoQ10, we will find no involvement of CoQ10 on glucose balance.
- In older Type II diabetics who have became refractory to their oral hypoglycemic medications, supplementing these individuals with CoQ10 will have an effect on glucose balance.
- Whenever the blood Q10 level is reduced to below 0.35 micrograms per milliliter, the body is not able to maintain glucose balance in older Type II diabetics.
- With Q10 supplementation raising plasma CoQ10, glucose balance is vastly improved.
Dr. Judy’s main point
It appears there is more to the body’s ability to handle glucose than insulin sensitivity and insulin secretion.
Until I talked with Dr. Judy, I had assumed that the research results show that Q10 supplementation is safe for diabetics, and I thought that that was a good thing since diabetics need Coenzyme Q10 to maintain heart health. I had not realized the need for Q10 supplementation to increase energy levels and to prevent or reverse a refractory response to diabetic drugs.
Earlier Coenzyme Q10 and diabetes studies
A 1999 study had shown that a supplementation of type II diabetics with 100 milligrams of Q10 twice daily that resulted in a three-fold rise in serum Q10 concentration did not interfere with the participants’ glycemic control. This finding meant that Q10 supplementation could be used as an adjunctive therapy in diabetic patients diagnosed with heart failure (2).
A second 1999 study had documented the supplementation of type I diabetics with 100 mg of Coenzyme Q10 for three months without any obvious risk of hypoglycemia or other unfavorable effects (3).
In 2002, a study involving the supplementation of type II diabetics with 200 milligrams of Q10 daily for 12 weeks had shown that Q10 supplementation may lead to improvements both in blood pressure and in long-term glycemic control (4).
All of these studies – Eriksson, Henriksen, and Hodgson – were good solid randomized, double-blind, placebo-controlled studies.
Sources:
- Cederberg H1, Stančáková A, Yaluri N, Modi S, Kuusisto J, Laakso M. (2015, Mar 10). Increased risk of diabetes with statin treatment is associated with impaired insulin sensitivity and insulin secretion: a 6 year follow-up study of the METSIM cohort. Diabetologia. [Epub ahead of print]
- Eriksson JG1, Forsén TJ, Mortensen SA, Rohde M. (1999). The effect of coenzyme Q10 administration on metabolic control in patients with type 2 diabetes mellitus. Biofactors;9(2-4):315-8.
- Henriksen JE, Andersen CB, Hother-Nielsen O, Vaag A, Mortensen SA, Beck-Nielsen H. (1999, Apr). Impact of ubiquinone (coenzyme Q10) treatment on glycaemic control, insulin requirement and well-being in patients with Type 1 diabetes mellitus. Diabet Med.;16(4):312-8.
- Hodgson, J. M., Watts, G. F., Playford, D. A., Burke, V., & Croft, K. D. (2002). Coenzyme Q10 improves blood pressure and glycaemic control: a controlled trial in subjects with type 2 diabetes. European Journal Of Clinical Nutrition, 56(11), 1137-1142.
- Judy, William. (2015, Mar). Private communication.









Leave A Comment